Are you one of the 77% still in denial?
Surveys by the American Heart Association show that only 50% of women know that heart disease is the leading cause of death. Yet only 13% said it was THEIR greatest risk. Are you one of the 77%?
For over 22 years, I have been trying to educate women on this truth, yet why the incredible disconnect? Perhaps you can guess – breast cancer can impact body image, sexuality, and self-esteem. Many women know at least one friend or family member that has had breast cancer. However, heart disease is silent and may not reveal itself until post-menopausal years. With that said, statistics show that more and more young women are dealing with heart disease!

This 40-year-old’s story
Jill was a beautiful, happily married, mid-executive mother of two. I met her when I was fresh out of graduate school and when she was in the Coronary Care Unit after her first heart attack. As a busy working mom of a thirteen-year-old son and a two-year-old daughter, she hustled to get everything done around the house on a Saturday morning. Like many moms of young toddlers trying to multi-task under the requirements of childcare and housework, she was vacuuming while holding her little girl. She was very sweaty and fatigued, but she thought she was just worn out from the work week.
As the afternoon progressed, she became nauseous and had mild pain in her right arm. Several hours went by before she decided to go to the ER. She brushed her symptoms aside all day. After all, typical heart attack symptoms are chest pain radiating down the left arm – for men. She didn’t have chest pain, and she was a 42-year-old woman. Because of those facts, she was sent home with recommendations to take it easy. Her fatigue, nausea, and now lightheadedness worsened through the night. Then the chest pain came, and back to the ER she went. The ER staff doubted it was a heart attack for the same reasons as before, her youth and her gender, so she waited for two hours before receiving an EKG and cardiac enzymes, which confirmed her heart attack.
Unfortunately for Jill, the delay ruled out the option for clot-busting drugs and increased the extent of damage to her heart. As Jill began to recover, she was discharged from the ICU and, after a few days, was sent home. She did not get a heart catheterization or even Cardiac Rehab, again, because she was young. Six weeks later, Jill suffered her second heart attack. Six weeks after that, she had emergency cardiac bypass surgery.
Why did this happen? Why the disparity in treatment? I’ll cover the disparity between men and women in more detail, but first, let’s review some of the stats.
Heart disease is still the leading cause of death for men, women, and people of most racial and ethnic groups in the United States. In fact, someone has a heart attack every 40 seconds. For our readers worldwide, the World Health Organization now states that heart disease is the number one killer globally.
The Gender Gap
Heart disease is the leading cause of death for women in the United States, killing 299,578 women in 2017—or about 1 in every 5 female deaths. Women are NOT small men in the disease process (pathogenesis), presentation (typical symptoms), prevention, diagnosis, and even treatment of Coronary Artery Disease (CAD). Unfortunately, only 56% of women recognize heart disease as their number one killer.
Due to a very successful media campaign, women are most concerned about breast cancer or some condition that causes immediate crises, such as hormonal symptoms and weight gain. Don’t be fooled; this is not just a problem for menopausal women. Thomas Sydenham, an English Physician (1624-1689), nailed it when he said, “A man is as old as his arteries.” That goes for women, too.
Women are unaware that even by age 20, they are already laying down significant plaque in their arteries. In our thirties, the plaque is even thicker, making us more susceptible to having a heart attack. As the plaque gets thicker and the inside edge of the vessel gets more rugged, platelets get aggravated and eventually will begin to form a clot. If a woman has gestational diabetes, hypertension from pregnancy, preeclampsia, or an autoimmune condition, her risks skyrocket.
Menopause brings another significant rise in women’s risk, as estrogen’s heart-protective effects are very low or even waning. As estrogen drops, you can experience not just hot flashes but changes in the walls of blood vessels that may cause plaque and cause blood clots to form. Additionally, estrogen depletion may cause changes in your levels of fats (lipids) in the blood. The Lousy LDL/low-density lipoproteins (cholesterol) may rise, and the Healthy HDL/high-density lipoprotein may drop, which exacerbates the build-up of fat and cholesterol that may contribute to a heart attack. Clotting factors, specifically fibrinogen, may also increase with low estrogen levels, further contributing to blood clot formation.
Over the years, there has been incredible controversy about using hormone therapy during and after menopause. While I will write another article on hormone balance, let me clarify that there is a significant difference between synthetic HRT (hormone replacement therapy) and BHRT (bioidentical hormone replacement therapy). Some estrogen therapy has been shown to be very beneficial during menopause, with the rule of treatment always being the lowest dose for the shortest duration of time. This is something that you should discuss with your doctor, taking into consideration your family history, genetics, diet, and lifestyle.
Now, let’s look at the difference in the disease process (Pathophysiology) between genders.
The Disease Process
Comparing the difference between men and women in how we gain weight to the cardiovascular disease process proves to be a very powerful analogy.
Men usually gain their weight in one spot – the belly! The plaque may look like a “pimple or a sore in men’s coronary artery.” Women, on the other hand, tend to gain weight from head to toe. Their coronary disease is also spread out more diffusely and into the tiny tips of the vessels.
Detailed studies of the arteries of women who died of heart attacks have found that the disease often looks much different in women in another way. “In men, it’s like a sore, like a pimple, that breaks and leads to the formation of a blood clot that causes a heart attack,” said Renu Vermani of the Armed Forces Institute of Pathology in Washington. “In women, we don’t see this pimple. We see erosion. It’s a malformation—like a scab, like a scar.” Vermani speculates that when arteries spasm, the innermost lining (called the endothelium) momentarily rubs against itself. “Over time, that causes it to erode,” he said. “The endothelium is disturbed, eroded, which leads to clot formation.” This, in turn, is the onset of a heart attack.
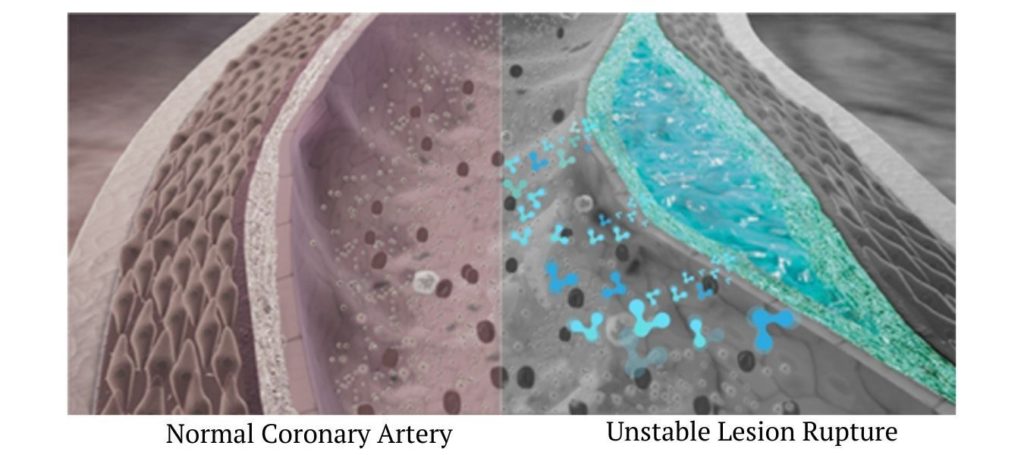
Because of the differing disease process, typical assessment or diagnostic tools, like an angiogram, may show no evidence of disease in a woman with significant disease. Recent studies have shown that it may take an MRI to show “ischemia” or lack of oxygen to a woman’s heart. The angiogram may come back completely “normal,” yet her heart is starving for oxygen!! With this in mind, the typical interventions that work well for men (Stents and Bypasses) may not be as effective or even an option for women.
In addition to the different disease processes, women experience different symptoms, as was the case for Jill. Whereas men typically have chest pain or “angina” that feels like an elephant sitting on his chest, women often experience fatigue and nausea, vomiting or sweating, and/or palpitations (a fast heartbeat). You can see why many women doubt they’re having a heart attack. If they get discomfort, it’s often in the neck, jaw, throat, and even the upper abdomen or back. These symptoms may happen when you are resting or when you are doing regular daily activities.
My intent in sharing this info is to educate and empower all of us, regardless of gender, to take better care of our hearts. Clearly, prevention is paramount, especially for women. You may be saying right now, “For heaven’s sake, how can I determine if I’m really having a heart attack or the flu?” Good question! It’s difficult for women. Personally, in my opinion, it’s essential to know your numbers, your family history, and your genetic risks, and employ the heart-healthy strategies recommended below.
The best way to “rule out” a heart attack is to get blood work done to measure cardiac enzymes (which rise during a heart attack) and to get a scan if you experience symptoms that concern you or match what I’ve described above. Stop if you’re exerting yourself, and take some slow deep breaths. Then proceed to the ER to get your blood drawn, an EKG, and perhaps more extensive scans.
Stay tuned for next week as I demystify hormones and heart health. Hormones in your 30’s & 40’s DO impact your heart health or risk of disease!

